By Christina M. Seluzicki, MBE, Eugenie Spiguel, MSN, ANP-BC, and Jun J. Mao, MD, MSCE
Sleep disturbances such as insomnia are prevalent and persistent among cancer survivors and diminish quality of life. Because of adverse effects such as continued sleep difficulty, memory disturbances, and falls associated with associated with conventional medications, many patients prefer nonpharmaceutical options to address their insomnia.
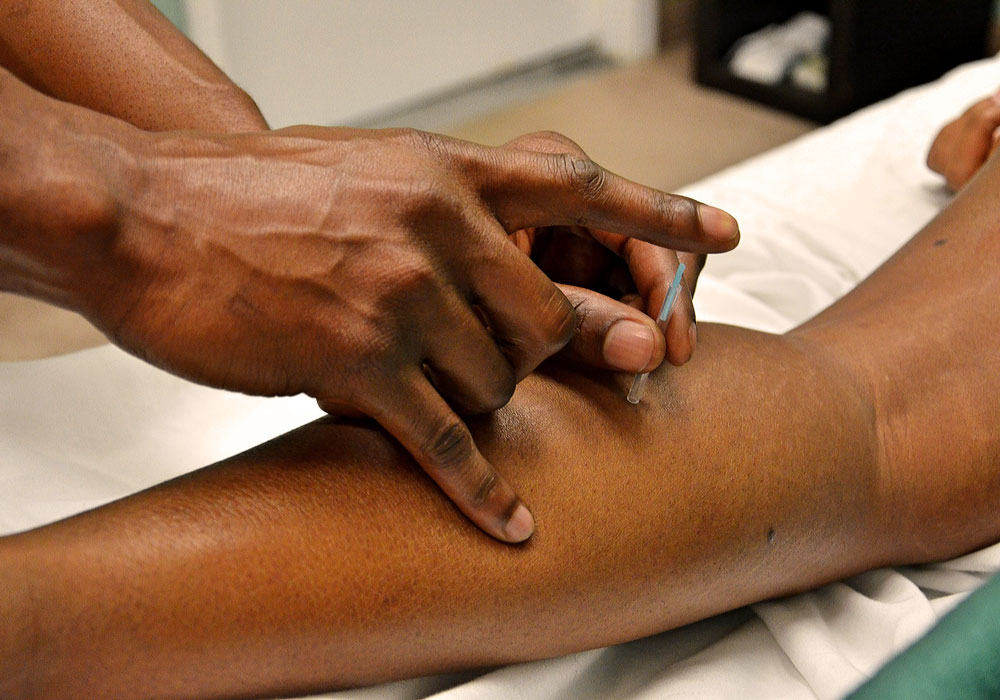
Two currently available approaches are acupuncture and cognitive-behavioral therapy for insomnia (CBT-I). Acupuncture involves stimulating predetermined points with fine needles, and CBT-I is a multimodal intervention specifically designed to address insomnia. Both have been shown to be effective, although the evidence for acupuncture in oncology settings is low. Also, their comparative effectiveness is not known.
The CHOICE Study
The Patient-Centered Outcomes Research Institute (PCORI)-funded Choosing Options for Insomnia in Cancer Effectively (CHOICE) study evaluated the relative efficacy of acupuncture versus CBT-I for decreasing insomnia severity in cancer survivors. Researchers randomly assigned 160 patients who had finished active treatment to receive one 60-minute and nine 30-minute acupuncture treatments or one 60-minute and six 30-minute CBT-I sessions over eight weeks. The primary outcome was patient-reported insomnia severity measured by the Insomnia Severity Index, a validated measure to assess the impact on daytime functioning and associated distress levels.
Although findings indicated that CBT-I was more effective than acupuncture (p < 0.001) overall, both treatments resulted in clinically meaningful reductions in insomnia severity (acupuncture: –8.31 points, 95% confidence interval = –9.36 to –7.26; CBT-I: –10.91 points, 95% confidence interval = –11.97 to –9.85). Furthermore, the reductions were sustained at the three-month follow-up. Interestingly, patients who had baseline pain, were women, were non-white, and had lower education received similar benefits from acupuncture and CBT-I for their insomnia. Future studies are required to confirm the variations and guide more personalized treatment for sleep issues.
What Oncology Nurses Need to Know
Insomnia is a debilitating symptom that many survivors experience. But given the multiple competing interests during a clinical oncology encounter, treating insomnia may not be a priority. When it is identified, sedative medications are typically the first line of treatment. Although they may be appropriate for short-term use in some populations, sedatives are associated with adverse events and do not effectively treat insomnia. Patients often become dependent and continue to have difficulty sleeping even while taking them. Better options are needed to address this serious disorder.
CBT-I and acupuncture are two safe strategies that have been shown to mitigate insomnia in the CHOICE study. Given the robust evidence for CBT-I, it should be the first line of treatment. However, few patients and oncology clinicians are aware of CBT-I’s benefits and access to qualified CBT-I therapists is limited. Acupuncture is also a good option for patients who have pain, prefer that treatment modality, or for whom CBT-I is not available.
Specific recommendations about these treatments are being formulated based on discussions from Sleeping Well After Cancer: Translating Patient-Centered Research Into Practice, a workshop held as part of the Society for Integrative Oncology’s 2019 International Conference and also funded by PCORI. The recommendations will help provide personalized insomnia treatments for cancer survivors with insomnia.
Oncology nurses have a critical role in helping patients identify insomnia and making them aware of evidence-based nonpharmacologic treatments. Ultimately, sleeping well will help improve quality of life and recovery for many patients with cancer.