Latest Headlines
- Nurse–Engineer Collaboration Creates Innovative Solutions to Healthcare Challenges
- Biomarkers for Persistent HPV May Predict Increased Cervical Cancer Risk
- ONS Virtual Conference Connects Nurses Around the World to Learn the Latest Evidence-Based Cancer Care
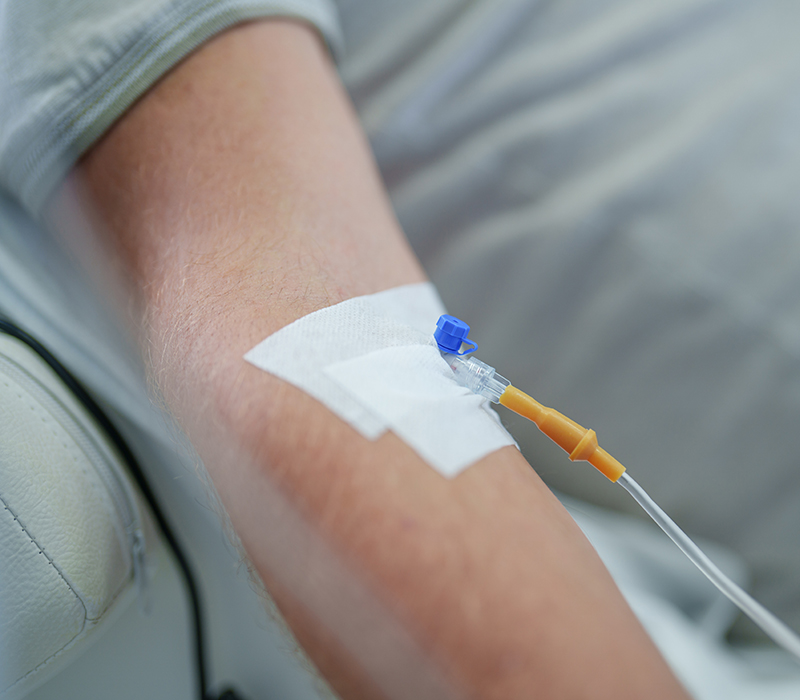
- Administration Considerations Amid the Large-Volume Subcutaneous Injection Revolution
Trending Topics
ONS Congress® News
- Peer Groups Offer a Safe Space for Oncology Nurses to Share Lived Experiences May 29, 2024
- Nurse Residency Programs Improve New Graduate RNs’ Transition to Clinical Practice May 22, 2024
- Infusion Center Rotations Help Inpatient Oncology Nurses Maintain Chemo Competency May 15, 2024
- Upskilled Medical Assistants Can Improve Quality and Efficiency of Cancer Care May 08, 2024
- Electronic Huddles Support Interprofessional Communication in the Ambulatory Care Setting May 01, 2024
Our Spirit. Our Practice.

Storytelling, which has benefits for nurses’ own well-being as well as their relationship with their patients, creates a social connection that fosters a sense of community and mutual support in the storyteller and listener. Inspired by ONS’s annual storytelling session at ONS Congress®, the Midwest Region Oncology Nursing Grand Rounds at Advocate Health hosted a special oncology grand rounds on nurse storytelling.