Multiple endocrine neoplasia type 1 (MEN1) is a rare autosomal dominant genetic disease affecting about 1 in 30,000 people. Pathogenic variants in the MEN1 gene are associated with benign and malignant tumors in the parathyroid glands, pituitary gland, pancreas, duodenum, and stomach.
The MEN1 gene provides instructions for producing the tumor suppressor protein menin. Loss of functional menin allows cells to divide too frequently and may lead to the formation of tumors, particularly in endocrine tissues. Approximately 10% of MEN1 variants are de novo.
Symptoms and Malignancies
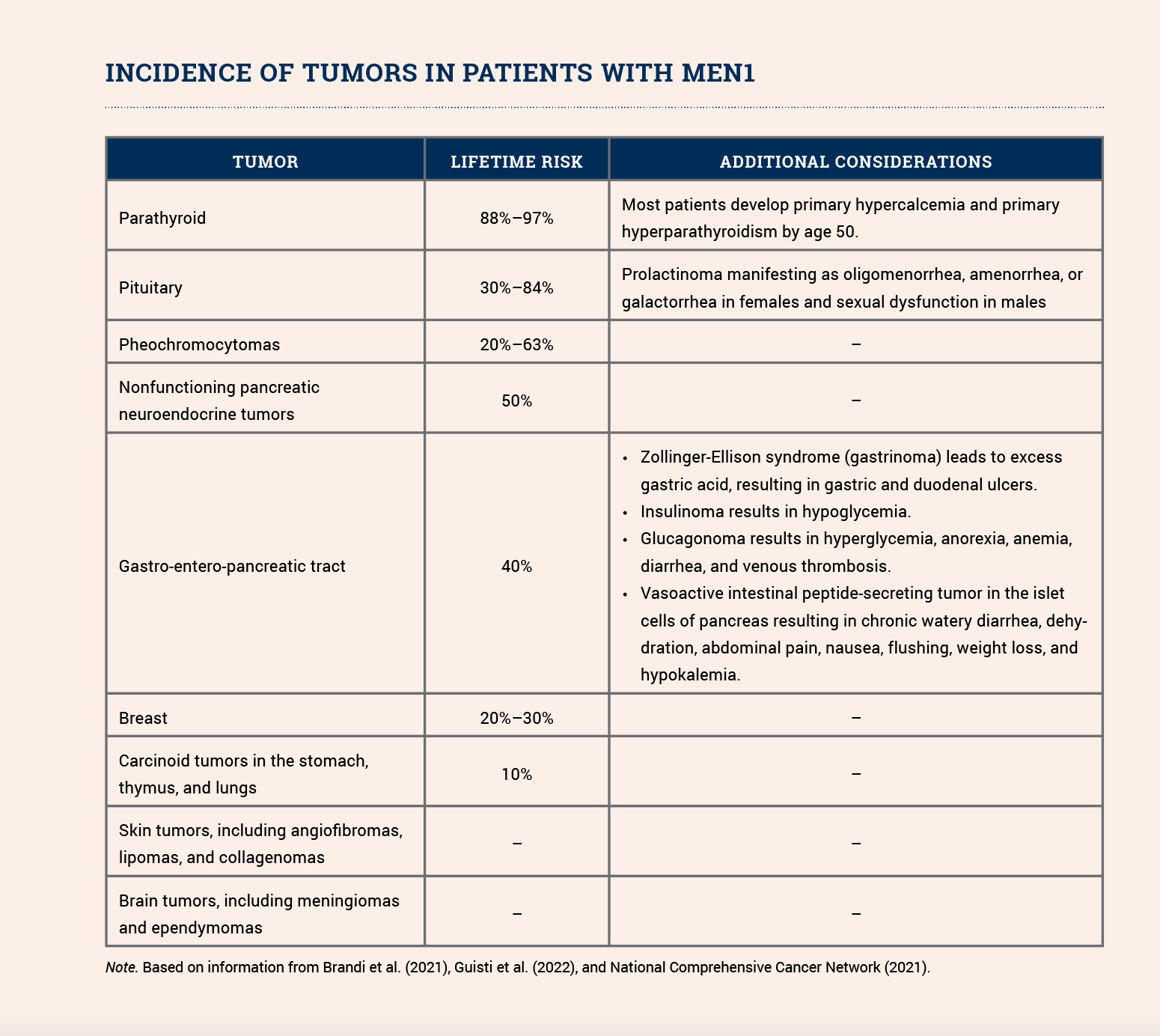
Individuals with an MEN1 pathogenic variant are at increased risk for developing benign and malignant tumors (see sidebar).
The penetrance (expression) of MEN1 symptoms is approximately 50% by age 20 and 95% by age 40. The diagnosis is clinically suspected by the combined occurrence of two or more of endocrinopathies. Mortality is often related to malignant neuroendocrine tumors.
Prevention and Early Detection
Ideally, people with a pathogenic MEN1 variant are managed by an interprofessional team that is familiar with its multiple complications. Complex recommended screening includes:
- Annually starting at age 5:
- Serum prolactin
- Magnetic resonance imaging (MRI) of the head
- Serum glucose, insulin, and proinsulin
- Annually starting at age 8:
- Serum concentrations of ionized or albumin-corrected calcium
- Serum parathyroid hormone
- Fasting and meal-stimulated pancreatic polypeptide
- Starting at age 20:
- Abdominal and chest computed tomography or MRI every two to three years
- Fasting serum gastrin annually
- Endoscopic ultrasound every three years
- Dermatologic examination annually
- Starting at age 30: annual breast cancer surveillance with mammography and breast MRI/breast ultrasound
Risk Reduction
Parathyroidectomy is the risk-reduction method of choice, but evidence is conflicting about whether to perform subtotal (less than 3.5 glands) or total parathyroidectomy and whether surgery should be performed at an early or late disease stage. Adults should have the surgery to prevent serious bone complications.
Thymectomy may prevent thymic carcinoid tumors and can be considered at the time of parathyroid neck surgery, particularly in smokers and individuals with a family history of thymic carcinoma.
Implications for Nurses
A primary nursing responsibility for MEN1 is providing ongoing psychosocial support and education on symptom identification and the importance of ongoing screening to detect tumors early, intervene accordingly, and improve prognosis. Individuals with MEN1 have a decreased life expectancy because of the presence of multiple tumors.
Smoking increases the risk of carcinoid tumors in MEN1. Nurses should encourage smoking cessation and help patients enroll in programs to quit.
The identification of a pathogenic MEN1 variant in a patient has implications for family members because first-degree relatives have a 50% risk of developing the syndrome. Patients with two or more symptoms should be referred to a genetics professional for MEN1 testing, which is recommended around age 3.






