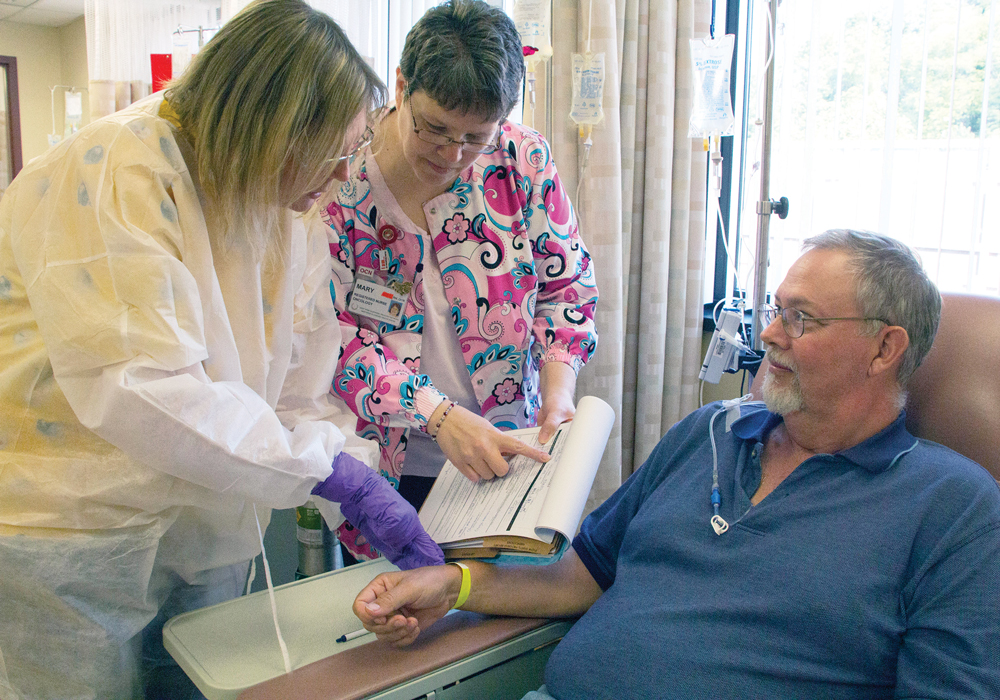
The elements of an oncology unit are often very similar from location to location—the crescendo of plastic wheels clicking across brightly shined linoleum, beaming fluorescent lights that flicker to life when switched on, mounted fountains of cool hand sanitizer gel. But although oncology units have many similarities, clear differences exist as well.
A recent discussion on the ONS communities centered around the process for delivering chemotherapy to an oncology unit. After the chemotherapy is prepared, does the pharmacist drop it off in a locked medicine room? Is it picked up by an administering nurse? Is it left at the nurses’ station? It’s a seemingly simple question, but the answers can have a great impact on patient safety and safe handling procedures.
Proper Chemotherapy Storage and Delivery
Medication errors are often life threatening, especially when involving chemotherapy agents. The proper storage and delivery of chemotherapy is vital to patient safety, and these processes can contribute to correct administration for every patient. This, coupled with two-RN verification and existing safety standards, can prevent dangerous medication errors from practice.
The Joint Commission, as part of its accreditation requirements, indicates that all chemotherapy should be stored in a locked medication area. Safety issues also exist with possible surface contamination to nonhazardous drugs, so the Joint Commission does not recommend storing chemotherapy and other hazardous agents near any other medications.
Furthermore, the 2016 ONS/ASCO Chemotherapy Administration Standards indicate that all intrathecal chemotherapy must be prepared and stored separate from other medications and treatments. It should be labeled with a unique identifier and must only be delivered to the patient with other medications intended for administration into the central nervous system (Standard 3.14).
By storing chemotherapy in designated, locked medication areas, nurses are able to separate hazardous drugs from nonhazardous drugs, verify medication dosing at multiple checkpoints in the process of administration, and ensure intrathecal medications are kept apart from intravenous chemotherapy agents to avoid fatal errors.
Advocating for Patient Safety
If you realize your institution isn’t adhering to current safety standards, consider starting a dialogue with your administration, charge nurse, and fellow colleagues. Identifying problems in practice is just the first step. Offering evidence-based literature and standards can help spur change. Consider approaching safety issues from an interprofessional viewpoint as well to ensure all voices on the team are heard.
Oncology nurses have a unique perspective when it comes to the patient experience. They’re continually called on to advocate for their patients and identify safety gaps in practice. Don’t hesitate to let your voice be heard.