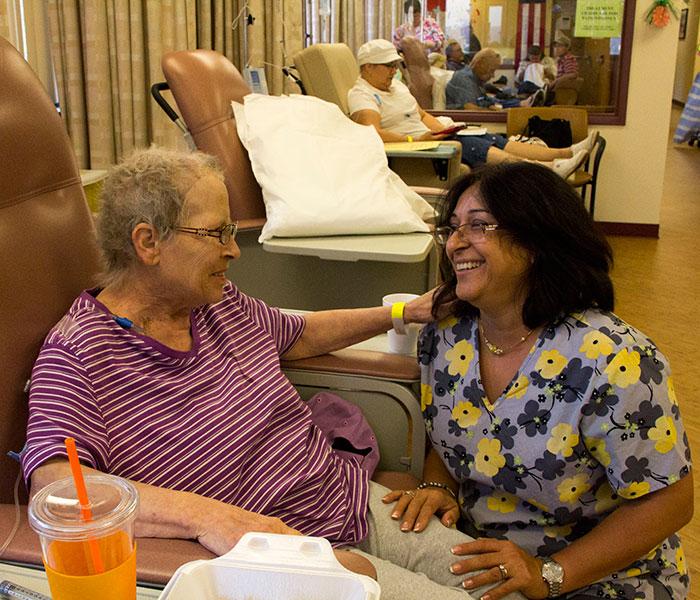A smile is universal across all cultures. It helps to break down language barriers. A smile is contagious. A smile can be heard and felt over the phone. A smile is not taught, it is simply part of our humanity. Babies smile in the womb. Smiling reduces stress hormones and releases endorphins physiologically helping one feel better. Oncology nurses know the power of a smile.
I just spent three days in an ICU at my father-in-law’s side. He miraculously survived a ruptured abdominal aortic aneurysm. It had been a long time since I’d been with a family member in the hospital. For a while now, I’ve wanted to write about the power of a smile, and the impact of an oncology nurse’s kind tone on the patient. The experience I just went through gave me the nudge I needed.
When my father-in-law was moved into the ICU, the first nurse he had made an impression on me, one I’ll never forget. She appeared to be an experienced nurse and was clearly skilled at her job. Unlike most ICU patients, my father-in-law was awake and alert. Perhaps she was burned out or experiencing compassion fatigue, but she was direct and almost stern when talking to my father-in-law. She did not smile and there was no tenderness.
My father-in-law was in tremendous pain, and the surgeon did not want him to have pain medicine because his blood pressure was dangerously low. I understood that, but my father-in-law, who was in agony, did not. At one point, another nurse came in to assist the primary nurse as my father-in-law was vomiting and needed to be suctioned. The assisting RN smiled at my father-in-law, said comforting words, and acknowledged his pain. I saw my father-in-law respond to this kindness and he immediately smiled. It was amazing.
His pain persisted. This nurse, however, was doing more than providing skills, she was comforting her patient with compassion. My father-in-law responded with a slightly relaxed face and became less agitated. I witnessed him over the next three days when he had a smiling nurse or aide. He responded more positively, and his impressions of that caretaker were that they were “good at their job.” He hoped he would have that staff member again the next day. To the patient, it did not matter how technically skilled the individual was at their job, it was how they interacted with him.
Over the three days I was there, I had experiences with nurses snapping at me when I asked what pain medicine he was getting and at what dosage. I had them tell me his blood pressure was “a little low” when it dropped to 67/45. As my father-in-law was in pain and vomiting, I cringed as the nurse pushed the morphine and then ten minutes later gave the Zofran. Physicians and nurses did not want to share lab numbers. They spoke so vaguely regarding lab results and plan of care that eventually the family requested a meeting with the physician to clarify information.
This was all such a surprising contrast for me. Oncology nurses are constantly working to educate patients and family members. We hand out lab results to patients, compare it to previous lab work, and we discuss the differences. We are constantly attempting to manage pain and nausea, all the while, educating the family and patient about what we are doing.
Above all else, we try to use kind tones, and smile when appropriate in order to connect in ways that are therapeutic to our patients. I don’t want to become a nurse that is just going through the motions and forgets the nurturing side of nursing. I’m proud to be part of the oncology nursing profession that understands and utilizes the amazing power of a smile!
Mother Teresa said: “I will never understand all the good that a simple smile can accomplish.”