Strategies to Promote Safe Medication Administration Practices
Medication administration is a high-risk process that requires critical thinking, efficient decision-making, attention to detail, and a foundational knowledge of basic pharmacology. The process is not a single task but a cascade of events that include handling, ordering, preparing, dispensing, administering, and monitoring. Although nurses’ involvement varies at each phase, the risk for errors always exists, and consequences can have a lifelong impact (https://www.npr.org/sections/health-shots/2022/03/25/1088902487/former-nurse-found-guilty-in-accidental-injection-death-of-75-year-old-patient) on patients, families, and healthcare workers. Nurses can use the following strategies in their responsibility as the last line of defense for safe medication administration.

Make a List and Check It Twice
Chemotherapy orders’ multistep review and verification process has been a mainstay of the American Society of Clinical Oncology/ONS Chemotherapy Safety Standards (https://www.ons.org/ascoons-chemotherapy-administration-safety-standards) since their inception in 2009. Create clarity and ownership by reviewing and understanding the various checkpoints (https://doi.org/10.1188/17.ONF.31-43) and identifying who in your setting’s workflow is responsible at each phase (https://doi.org/10.1188/17.ONF.31-43) of the process. Consider ways to integrate standardized checklists, templates, or tools into the documentation workflow to consistently complete independent dual verification of chemotherapy orders. (See the ONS Huddle Card™ series (https://www.ons.org/learning-libraries/huddle-cards).)
Take a Time Out
Assess the environment in which you are conducting independent dual verification: Do you have a dedicated space and time to review orders? Are you free from distractions or competing priorities? Are the necessary references and tools available to complete accurate drug calculations? Consider borrowing a page from our surgical nurse colleagues to set up a treatment verification “time out” process or zone (https://doi.org/10.1097/ncq.0b013e3181ce3ae4) to signal that a nurse should not be interrupted during their critically important task.
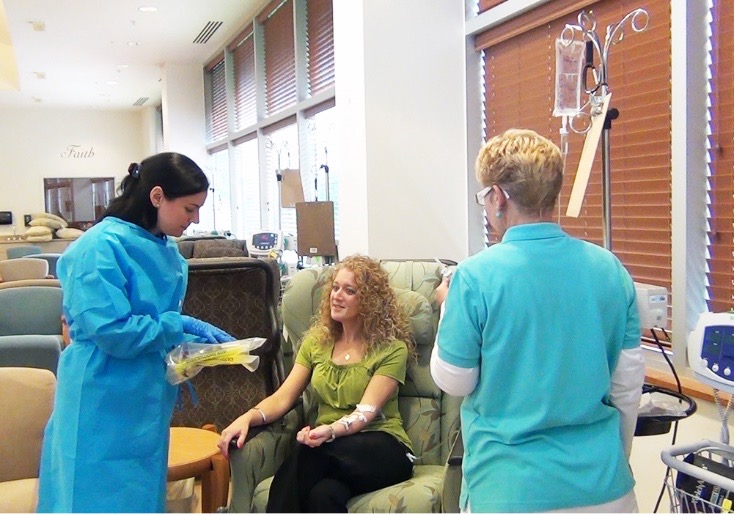
Involve Your Patients
You encourage your patients to be active and engaged members of their own care team, communicate their preferences, and share in decision-making. Extend that responsibility to include participating in the safe administration of their medications. Using the Joint Commission’s Speak Up! resources (https://www.jointcommission.org/-/media/tjc/documents/resources/speak-up/medicine_mistakes_brochure-5-15-2020.pdf) as a foundation, empower your patients to voice any questions or concerns at any point during the medication administration process with the following teaching points:
- Make sure we validate your identity by asking you to state your name and date of birth or checking your wristband.
- If you are concerned you are receiving the wrong medication, speak up immediately and ask for clarification.
- We will tell you each medication’s name, the dose, what it’s used for, and how long its infusion will take. If we don’t tell you, ask!
- Learn the full names of your medications and keep a current list. Ask whether the medication or treatment regimen is commonly called something else (such as a brand name versus generic or an abbreviation like “R-CHOP” or “FOLFOX”).
- Never be afraid to ask questions or for us to repeat information to ensure you understand.
Initiate Improvements
Review your setting’s order and drug verification procedures and consider whether these tools and techniques may offer an additional layer of safety. Connect with oncology nursing colleagues across the country on the ONS Communities (http://communities.ons.org/) to share your best practices and learn what others are doing. As oncology nurses, we have a never-ending responsibility to improve the safety of our work and must use every opportunity to do that
